For most people with a mental illness, employment is part of their recovery.
Most people with severe mental illness want to work. Approximately 2 of every 3 people with mental illness are interested in competitive employment [1-8] but less than 15% are employed [9-12].
Individual Placement and Support (IPS) supported employment is evidence-based.
IPS helps people join the competitive labor market [13,14]. IPS is three times more effective than other vocational approaches in helping people with mental illness to work competitively [15-18]. IPS has been found effective for numerous populations in which it has been tried, including people with many different diagnoses, educational levels, and prior work histories [19]; long-term Social Security beneficiaries [20]; young adults [21,22]; older adults [23]; veterans with post-traumatic stress disorder [24] or spinal cord injury[25]; and people with co- occurring mental illness and substance use disorders [26]. To date, we have not discovered a subgroup for which IPS has not been effective.
IPS is cost-effective.
Severe mental illness is a leading contributor to the global burden of disease [27,28] and constitutes the largest and fastest growing group of beneficiaries in Social Security disability programs [29,30]. Once on the disability rolls, less than 1% of beneficiaries per year move off of benefits to return to work [31-33]. By helping people with mental illness gain employment, especially young adults experiencing early psychosis, IPS can help forestall entry into the disability system and reduce Social Security expenditures [34-38].
IPS is an excellent investment, with an annual cost of $5500 per client in 2012 dollars [39,40]. Most clients enrolled in IPS receive more mental health services than IPS services [41-43]. IPS is cost-effective over the long term when mental health treatment costs are considered. Studies have found a reduction in community mental health treatment costs for people receiving supported employment services [44-48] and a reduction in psychiatric hospitalization days and emergency room usage by clients who receive supported employment [49-51]. Service agencies converting their day treatment programs to IPS have reduced service costs by 29% [45].
Over the long term, clients who return to work produce huge long-term savings in mental health treatment costs. A 10-year follow-up study of clients with co-occurring severe mental illness and substance abuse disorder found an average annual savings of over $16,000 per client in mental health treatment costs for steady workers, compared to clients who remained out of the labor market [52].
IPS improves long-term well-being.
People who obtain competitive employment through IPS have increased income, improved self-esteem, improved quality of life, and reduced symptoms [49,53-55]. Approximately 40% of clients who obtain a job with help from IPS become steady workers [56] and remain competitively employed a decade later [57,58].
IPS programs have a high rate of successful implementation and sustainability over time.
The IPS model is a common sense, practical intervention that appeals to clinicians, clients, and the general public [59,60]. Quality of IPS implementation is measured using a standardized fidelity scale [61]. Programs ordinarily achieve high fidelity implementation within one year’s time [62]. High fidelity IPS programs have excellent competitive employment outcomes [63,64]. IPS is relatively easy to implement with high fidelity, as shown in numerous implementation projects [20,42,62,65]. With adequate funding, committed leadership, and fidelity monitoring, [66] multi-site projects have successfully implemented IPS in over 80% of programs adopting this approach. IPS has been successfully implemented in both urban and rural communities [67,68]. Once implemented, most IPS programs continue indefinitely to offer quality services if adequate infrastructure remains in place. One study found 84% of 165 IPS programs implemented over the last decade were still providing services in 2012 [69].
Most Americans with severe mental illness do not have access to IPS.
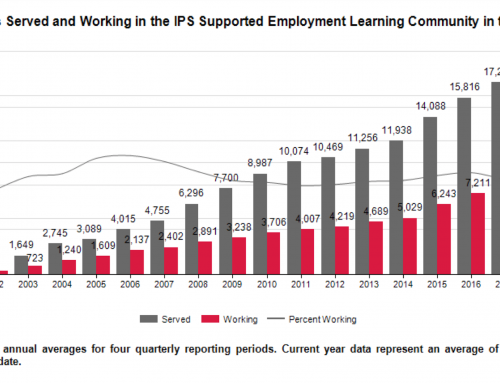
Despite the benefits of IPS, access to IPS is limited or unavailable in many communities. First the good news: the Dartmouth-Johnson & Johnson Learning Collaborative has grown to 138 programs in 14 states with two new international partners (Italy and the Netherlands) [69]. But only 2.1% of clients with severe mental illness in the U.S. public mental health system received supported employment in 2009 [70]. Similarly, during 2007, <1% of Medicaid patients with schizophrenia had an identifiable claim for supported employment [71]. Wider access to IPS would benefit people with severe mental illness, their families, taxpayers, and the general public.
References
- Bedell JR, Draving D, Parrish A, Gervey R, Guastadisegni P. A description and comparison of experiences of people with mental disorders in supported employment and paid prevocational training. Psychiatric Rehabilitation Journal 1998;21(3):279-283.
- Frounfelker RL, Wilkniss SM, Bond GR, Devitt TS, Drake RE. Enrollment in supported employment services for clients with a co-occurring disorder. Psychiatric Services 2011;62:545-547.
- McQuilken M, Zahniser JH, Novak J, Starks RD, Olmos A, Bond GR. The Work Project Survey: Consumer perspectives on work. Journal of Vocational Rehabilitation 2003;18:59-68.
- Mueser KT, Salyers MP, Mueser PR. A prospective analysis of work in schizophrenia. Schizophrenia Bulletin 2001;27:281-296.
- Ramsay CE, Broussard B, Goulding SM, et al. Life and treatment goals of individuals hospitalized for first-episode nonaffective psychosis. Psychiatry Research 2011;189:344-348.
- Rogers ES, Walsh D, Masotta L, Danley K. Massachusetts survey of client preferences for community support services: Final report. Boston: Center for Psychiatric Rehabilitation, 1991: 1-59.
- Watkins KE, Pincus HA, Paddock S, et al. Care for veterans with mental and substance use disorders: good performance, but room to improve on many measures. Health Affairs 2011;30:2194-2203.
- Woltmann E. Development and evaluation of a consumer-directed decision support system to support shared decision making in community mental health. dissertation: Dartmouth, 2009.
- Lindamer LA, Bailey A, Hawthorne W, et al. Gender differences in characteristics and service use of public mental health patients with schizophrenia. Psychiatric Services 2003;54:1407-1409.
- Pandiani J, Leno S. Employment of CRT clients: third quarters (Jan-Mar) of FY2000-FY2012. Waterbury, VT: Vermont Agency of Human Services, 2012.
- Rosenheck RA, Leslie D, Keefe R, et al. Barriers to employment for people with schizophrenia. American Journal of Psychiatry 2006;163:411-417.
- Salkever DS, Karakus MC, Slade EP, et al. Measures and predictors of community- based employment and earnings of persons with schizophrenia in a multisite study. Psychiatric Services 2007;58:315-324.
- Becker DR, Drake RE. A working life for people with severe mental illness. New York: Oxford University Press, 2003.
- Becker DR, Drake RE, Bond GR. Benchmark outcomes in supported employment. American Journal of Psychiatric Rehabilitation 2011;14:230-236.
- Bond GR, Drake RE, Becker DR. An update on randomized controlled trials of evidence-based supported employment. Psychiatric Rehabilitation Journal 2008;31:280-290.
- Bond GR, Campbell K, Drake RE. Standardizing measures in four domains of employment outcome for Individual Placement and Support. Psychiatric Services 2012;63:751-757.
- Drake RE, Bond GR, Becker DR. IPS supported employment: An evidence-based approach to supported employment. New York: Oxford University Press, 2012.
- Bond GR, Drake RE, Becker DR. Generalizability of the Individual Placement and Support (IPS) model of supported employment outside the US. World Psychiatry 2012;11:32-39.
- Campbell K, Bond GR, Drake RE. Who benefits from supported employment: A meta-analytic study. Schizophrenia Bulletin 2011;37:370-380.
- Frey WD, Drake RE, Bond GR, et al. Mental Health Treatment Study: Final Report to Social Security Administration (http://socialsecurity.gov/disabilityresearch/mentalhealth.htm). Rockville, MD: Westat, 2011.
- Bond GR, Drake RE, Campbell K. The effectiveness of the Individual Placement and Support model of supported employment for young adults: Results from four randomized controlled trials. International Early Psychosis Association 2012, San Francisco, CA.
- Rinaldi M, Killackey E, Smith J, Shepherd G, Singh S, Craig T. First episode psychosis and employment: A review. International Review of Psychiatry 2010;22:148-162.
- Twamley EW, Vella L, Burton CZ, Becker DR, Bell MD, Jeste DV. The efficacy of supported employment for middle-aged and older people with schizophrenia. Schizophrenia Research 2012;135:100-104.
- Davis LL, Leon AC, Toscano R, et al. A randomized controlled trial of supported employment among veterans with posttraumatic stress disorder. Psychiatric Services 2012;63:464–470.
- Ottomanelli L, Goetz LL, Suris A, et al. Effectiveness of supported employment for veterans with spinal cord injuries: results from a randomized multisite study. Archives of Physical Medicine and Rehabilitation 2012;93:740-747.
- Mueser KT, Campbell K, Drake RE. The effectiveness of supported employment in people with dual disorders. Journal of Dual Disorders 2011;7:90-102.
- Drake RE, Bond GR, Thornicroft G, Knapp M, Goldman HH. Mental health disability: An international perspective. Journal of Disability Policy Studies 2012;23:110-120.
- World Health Organization. World Health Report 2001. Mental health: New understanding, new hope. Geneva: World Health Organization, 2001.
- Danziger S, Frank RG, Meara E. Mental illness, work, and income support programs. American Journal of Psychiatry 2009;166:398-404.
- McAlpine DD, Warner L. Barriers to employment among persons with mental illness: A review of the literature. New Brunswick, NJ: Center for Research on the Organization and Financing of Care for the Severely Mentally Ill Institute for Health, Health Care Policy and Aging Research Rutgers, the State University, 2000: 1-49.
- Kennedy J, Olney M, Schiro-Geist C. A national profile of SSDI recipients and applicants: implications for early intervention. Journal of Disability Policy Studies 2004;5:178-185.
- Liu S, Stapleton D. How many SSDI beneficiaries leave the rolls for work? More than you might think. Disability Policy Research Brief 2010;10-01:1-4.
- SSA. 42 USC 1320b-19, Section 2(a)(8). 2009.
34. Drake RE, Skinner JS, Bond GR, Goldman HH. Social Security and mental illness:Reducing disability with supported employment. Health Affairs 2009;28:761-770. - Norman RM, Mallal AK, Manchanda R, et al. Does treatment delay predict occupational functioning in first-episode psychosis? Schizophrenia Research 2007;91:259-262.
- Krupa T, Oyewumi K, Archie S, Lawson JS, Nandlal J, Conrad G. Early intervention services for psychosis and time until application for disability income support: a survival analysis. Community Mental Health Journal 2012;DOI: 10.1007/s10597- 012-9496-z.
- Mental Health Commission of Canada. Changing directions, changing lives: the mental health strategy for Canada. Alberta, CA: Mental Health Commission of Canada, 2012.
- Cougnard A, Goumilloux R, Monello F, Verdoux H. Time between schizophrenia onset and first request for disability status in France and associated patient characteristics. Psychiatric Services 2007;58:1427-1432.
- Latimer E, Bush P, Becker DR, Drake RE, Bond GR. How much does supported employment for the severely mentally ill cost? An exploratory survey of high-fidelity programs. Psychiatric Services 2004;55:401-406.
- Salkever DS. Toward a social cost-effectiveness analysis of programs to expand supported employment services: An interpretive review of the literature. Rockville, MD: Westat, 2011.
- Cook JA, Lehman AF, Drake R, et al. Integration of psychiatric and vocational services: A multisite randomized, controlled trial of supported employment. American Journal of Psychiatry 2005;162:1948-1956.
- Herinckx H. Oregon Supported Employment Center For Excellence final evaluation report. Portland, OR: Regional Research Institute for Human Services, Portland State University, 2011.
- McGuire AB, Bond GR, Clendenning D, Kukla M. Service intensity as a predictor of competitive employment in an Individual Placement and Support program. Psychiatric Services 2011;62:1066-1072.
- Bond GR, Dietzen LL, Vogler KM, Katuin CH, McGrew JH, Miller LD. Toward a framework for evaluating costs and benefits of psychiatric rehabilitation: Three case examples. Journal of Vocational Rehabilitation 1995;5:75-88.
- Clark RE. Supported employment and managed care: Can they coexist? Psychiatric Rehabilitation Journal 1998;22(1):62-68.
- Latimer E. Economic impacts of supported employment for the severely mentally ill. Canadian Journal of Psychiatry 2001;46:496-505.
- Perkins DV, Born DL, Raines JA, Galka SW. Program evaluation from an ecological perspective: Supported employment services for persons with serious psychiatric disabilities. Psychiatric Rehabilitation Journal 2005;28:217-224.
- Schneider J, Boyce M, Johnson R, et al. Impact of supported employment on service costs and income of people with mental health needs. Journal of Mental Health 2009;18:533-542.
- Burns T, Catty J, White S, et al. The impact of supported employment and working on clinical and social functioning: Results of an international study of Individual Placement and Support. Schizophrenia Bulletin 2009;35:949-958.
- Henry AD, Lucca AM, Banks S, Simon L, Page S. Inpatient hospitalizations and emergency service visits among participants in an Individual Placement and Support (IPS) model program. Mental Health Services Research 2004;6:227-237.
- Rogers ES, Sciarappa K, MacDonald-Wilson K, Danley K. A benefit-cost analysis of a supported employment model for persons with psychiatric disabilities. Evaluation and Program Planning 1995;18:105-115.
- Bush PW, Drake RE, Xie H, McHugo GJ, Haslett WR. The long-term impact of employment on mental health service use and costs. Psychiatric Services 2009;60:1024-1031.
- Bond GR, Resnick SG, Drake RE, Xie H, McHugo GJ, Bebout RR. Does competitive employment improve nonvocational outcomes for people with severe mental illness? Journal of Consulting and Clinical Psychology 2001;69:489-501.
- Kukla M, Bond GR, Xie H. A prospective investigation of work and nonvocational outcomes in adults with severe mental illness. Journal of Nervous and Mental Disease 2012;200:214–222.
- Mueser KT, Becker DR, Torrey WC, et al. Work and nonvocational domains of functioning in persons with severe mental illness: A longitudinal analysis. Journal of Nervous and Mental Disease 1997;185:419-426.
- Bond GR, Kukla M. Is job tenure brief in Individual Placement and Support (IPS) employment programs? Psychiatric Services 2011;62:950-953.
- Becker DR, Whitley R, Bailey EL, Drake RE. Long-term employment outcomes of supported employment for people with severe mental illness. Psychiatric Services 2007;58:922-928.
- Salyers MP, Becker DR, Drake RE, Torrey WC, Wyzik PF. Ten-year follow-up of clients in a supported employment program. Psychiatric Services 2004;55:302-308.
- Dreher KC, Bond GR, Becker DR. The creation of the IPS-Q: A measure to assess knowledge of the Individual Placement and Support model. Psychiatric Rehabilitation Journal 2010;33:181-189.
- Swanson SJ, Becker DR, Drake RE, Merrens MR. Supported employment: A practical guide for practitioners and supervisors. Lebanon, NH: Dartmouth Psychiatric Research Center, 2008.
- Becker DR, Swanson SJ, Bond GR, et al. Supported Employment Fidelity Scale. Lebanon, NH: Dartmouth Psychiatric Research Center (http://www.dartmouthips.org), 2008.
- Bond GR, McHugo GJ, Becker DR, Rapp CA, Whitley R. Fidelity of supported employment: Lessons learned from the National Evidence-Based Practices Project. Psychiatric Rehabilitation Journal 2008;31:300-305.
- Bond GR, Becker DR, Drake RE. Measurement of fidelity of implementation of evidence-based practices: Case example of the IPS Fidelity Scale. Clinical Psychology: Science and Practice 2011;18:126-141.
- Bond GR, Peterson AE, Becker DR, Drake RE. Validating the revised Individual Placement and Support Fidelity Scale (IPS-25). Psychiatric Services 2012;63:758- 763.
- Becker DR, Drake RE, Bond GR, Nawaz S, Haslett WR, Martinez RA. A mental health learning collaborative on supported employment. Psychiatric Services 2011;62:704-706.
- Torrey WC, Bond GR, McHugo GJ, Swain K. Evidence-based practice implementation in community mental health settings: The relative importance of key domains of implementation activity. Administration and Policy in Mental Health and Mental Health Services Research 2012;39:353-364.
- Haslett WR, Bond GR, Drake RE, Becker DR, McHugo GJ. Individual Placement and Support: Does rurality matter? American Journal of Psychiatric Rehabilitation 2011;14:237-244.
- Peterson AE, Bond GR, Becker DR, Drake RE. Achieving high fidelity to supported employment: comparing programs in small and large communities. submitted.
- Becker DR. Unpublished data on IPS Learning Collaborative. Lebanon, NH: Dartmouth Psychiatric Research Center, 2012.
- SAMHSA. http://www.samhsa.gov/dataoutcomes/urs/urs2009.aspx, 2009.
- Brown JD, Barrett A, Ireys H, Caffery E, Hourihan K. Evidence-based practices for Medicaid beneficiaries with schizophrenia and bipolar disorder. Washington, DC: Office of Disability, Aging and Long-Term Care Policy, Office of the Assistant Secretary for Planning and Evaluation, U.S. Department of Health and Human Services, 2012.